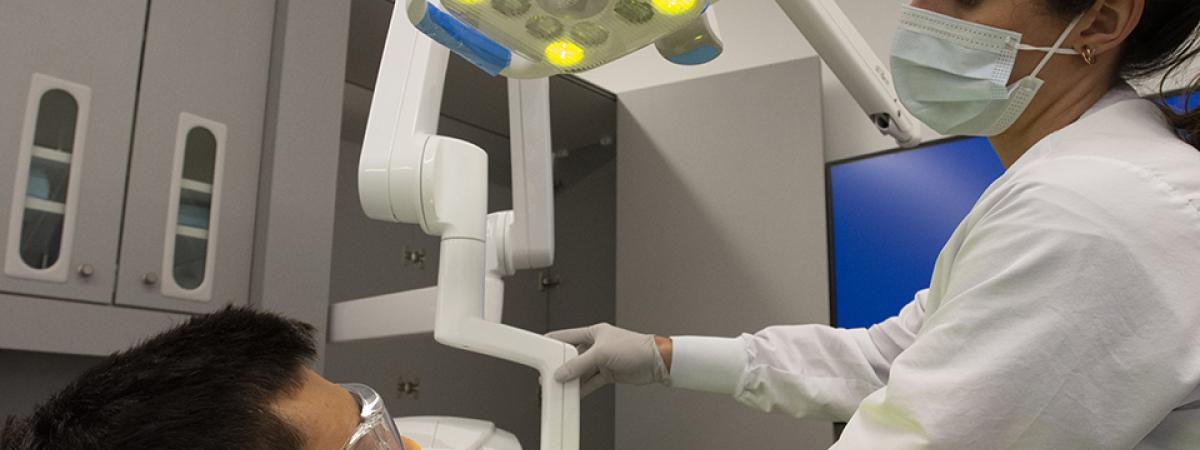
From long-standing programs such as the Provost Scholars, new pathways through the Gelfand STEM Center, our dental school, and beyond; we offer unique opportunities for K-12 students in our surrounding communities.
The Neighborhood Advisory Council is composed of community residents, CWRU students, and university and local representatives dedicated to promoting the community’s interests and building mutually respectful partnerships.

Our new interactive resource, “Collaboratory,” catalogs the university’s outreach programs and efforts so community members can stay informed on engagement activity and learn how to get involved. This is constantly being updated.

The CWRU Community Card allows residents of our surrounding communities to enjoy selected services and amenities provided by Case Western Reserve University and discounts from participating businesses.