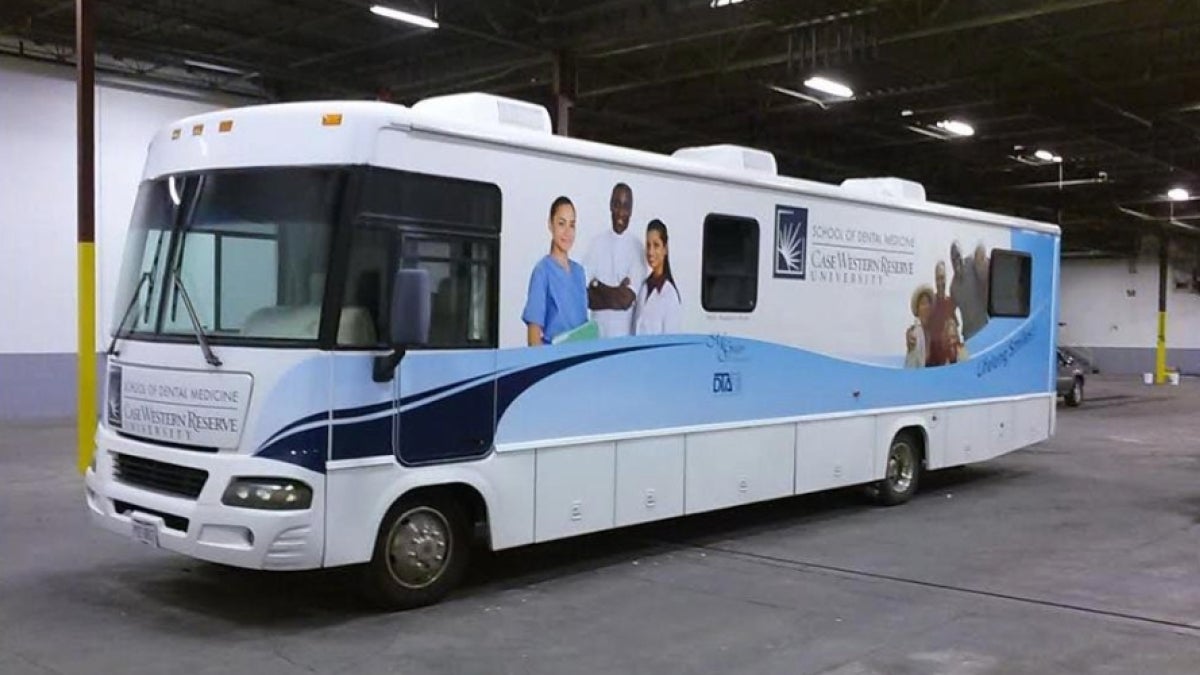
A different kind of dental visit
The School of Dental Medicine’s geriatric dental program is taking dental care in a new direction—and impacting both patients and students along the way.
The first thing fourth-year dental student Vihisha Bache noticed wasn’t the patient’s teeth—it was her hesitation.
Seated in a makeshift exam space inside a community center, an apprehensive woman gripped her walker and leaned back slightly, unsure of what would come next. She didn’t speak English, and no one on site understood her language, but she desperately needed dental care. So, Bache slowed down. She held up a dental instrument, demonstrated how it worked and mimicked each step of the procedure before performing it.
Gradually, the patient relaxed. By the end of the visit, she had been referred for follow-up care—and eventually connected with a provider who spoke her language.
But the challenges of the day didn’t stop with the language barrier. Bache wasn’t treating patients in the dental clinic. Instead, she was participating in Case Western Reserve University’s mobile geriatric dental program, part of its broader community dentistry initiative. The program, which brings care directly into neighborhoods across Northeast Ohio, treats patients who may never make it into a dental office—because of mobility challenges, transportation barriers, cost or fear—and gives fourth-year students firsthand experience treating them in real-world settings.
Taking dentistry on the road

The program itself was designed around a simple but powerful question: What happens when patients can’t access care on their own?
“The patient can’t get to me—so how do I get to my patient?” said Suparna Mahalaha, DDS (CWR ’98; DEN ’01; GRS ’04, public health), director of the geriatric dental program and associate professor of community dentistry. “That is the problem we need to solve, so that we can provide care to everyone in the community, not just the ones that can make it to the clinic.”
Originally launched in 2014, the initiative began with a fully equipped 38-foot mobile dental van, allowing students and faculty to deliver comprehensive care such as exams, X-rays, cleanings, extractions and dentures directly in community settings like adult day centers. Over time, however, the program has evolved. The original van, now aging and without a dedicated driver, is no longer in use. Until funds can be raised for a new van or a new driver can be hired, the team relies on portable equipment stationed at the various sites. While this allows the work—serving 100 to 200 patients each year—to continue, it has introduced new challenges that students experience firsthand.
“The van let us effectively take the clinic on the road,” Mahalaha explained. “Now, we have to get a little more creative with mobile dental equipment.”
Instead of being in dental chairs, patients are regularly seated in armchairs, wheelchairs or walkers, often unable to recline. Resources are limited, and even basic equipment such as suction or lighting may not function as smoothly as in a fixed operatory. For Bache, one of the biggest adjustments was learning to practice without the structure and convenience of a traditional clinic.
“We don’t have our nice units,” she said. “We have to think, ‘OK, I have like five tools, and I have to work with what I have.’ You have to be resourceful, think on your feet and really bend over backwards for these patients—literally and figuratively.”
That adaptability is one of the things the program aims to teach. Mahalaha emphasizes that working in a mobile or community setting pushes students to develop skills that go beyond technical proficiency.
“You don’t need this perfect dental office to be able to treat a patient,” she said. “You can go to the patient and you can still provide great care.”
Reimagining care

Working in nontraditional spaces with underserved populations also requires rethinking how care is delivered. With geriatric and special needs populations, treatment plans are rarely straightforward. Physical limitations, cognitive conditions and access to ongoing care all play a role in determining what is realistic. In some cases, that means choosing options that prioritize comfort and function over ideal clinical outcomes. For example, the dentist may extract a tooth instead of making plans that require follow-up care that the patient won’t be able to receive.
“Your first treatment plan is rarely going to be the best one in these situations,” Bache said. “A case may seem straightforward and there may be steps you would traditionally follow, but here you have to really take the patient and their situation into consideration.”
Yet even within those constraints, the impact of just being out in the community can be profound. Bache saw firsthand how even brief interactions can lead to meaningful change. During one outreach visit, she spent just a few minutes speaking with a father about his child’s dental health. Later, she encountered him again—this time in the clinic, having brought his son in for care. Experiences like those have reshaped her understanding of what dentistry can be.
“It was just such a simple five-minute conversation,” she said, “but clearly it made a huge impact. I feel like the conversation, the time and the patience that we show them is part of the treatment. I think that is half of the healing journey.”
Mahalaha has seen this dynamic play out countless times. She recalls a nursing home patient who had stopped eating and socializing because of pain from an ill-fitting denture. A quick adjustment—“it took less than 10 seconds”—allowed the patient to eat again, leave her room and reengage with others.
“It helped her quality of life,” Mahalaha said. “I didn’t do something wildly difficult, but I helped her in a significant way. We can make a big difference just by listening and meeting people where they are—both physically and emotionally. Patients face so many barriers to care and if we can help them overcome them, we want to do that.”
Lasting effects
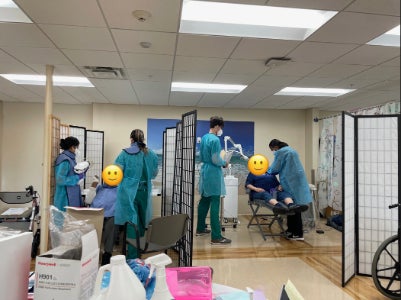
By bringing care directly into the community, the program helps bridge those gaps—while also giving students a glimpse of what their future roles as providers might look like beyond the clinic walls. For many, including Bache, the experience was transformative.
“It felt like we were really having our first taste of a real-life dentist job,” she said. “There’s a sense of independence that comes with working in these settings, balanced by the understanding that each patient encounter requires patience, empathy and flexibility.”
That combination has left a lasting impression. Although she plans to specialize in pediatric dentistry, Bache says her experiences with older adults have felt surprisingly familiar.
“In my culture, we say that children and the geriatric population become the same at some point,” she explained. “You come full circle. And I had that same fulfillment and enjoyment with the geriatric patients that I do with the pediatric ones. While I am going into pediatrics, I definitely now want to make community outreach a central component of my career.”
In many ways, that reflects the program’s broader goal—not just to treat patients, but to shape the kind of dentists the dental students will become. By challenging them to step outside traditional models of care, students are encouraged to think differently about access, responsibility and outcomes. It’s important, Mahalaha emphasized, to remember that there are many ways to practice meaningful, impactful dentistry.
For Bache, that realization came not in CWRU’s state-of-the-art clinic, but in moments like the one with her hesitant patient. By slowing down and making a connection, she found ways to provide care despite the obstacles. It’s a lesson she knows will stay with her long after graduation.
“I don’t think I’ll ever forget my time in the geriatrics program,” she said. “I learned so much about providing care with compassion and resourcefulness. I think the experience was just as impactful for me as it was for the patients.”




