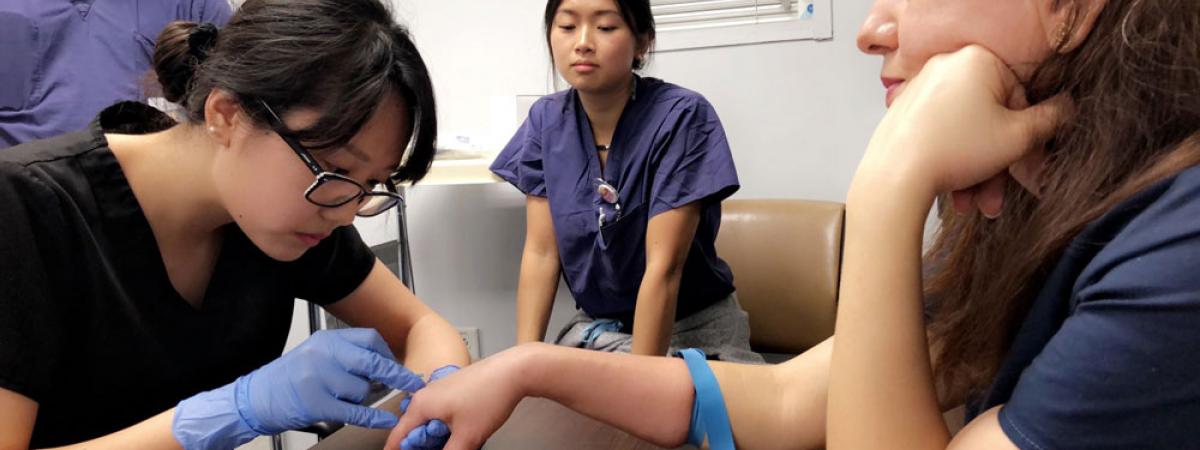
In 2009, the Master of Science in Anesthesia Program at Case Western Reserve University underwent a major curricular restructuring with a specific focus on improving and advancing our didactic and simulation curriculum.
Today, our didactic and clinical courses work hand-in-hand with our simulation laboratory training, which gives students the space to apply their skills in a mock operating room where they can learn from their mistakes, reflect on their practice, and collaborate with their peers. The simulation training is innovative in its integration of clinical and didactic skills, and offers opportunities for physicians and faculty to give individualized attention to students during hi-fidelity simulations.
Furthermore, the overarching goals of the curriculum not only reflect the mission of the program—to train the best anesthetists in the world— but also integrate key clinical practicum and student learning objectives that prepare students for success in the operating room and beyond.
MSA Program First Year: Basic Science and Clinical
First Year Coursework
The first year provides students with a broad education in basic science disciplines with a focus on the practice of anesthesiology. Students begin with the fundamental aspects of anesthesia, including basic physiology and pharmacology, and the skills involved in the administration of anesthesia and associated invasive and non-invasive monitoring. This is the thrust of our didactic curriculum, which is the primary focus of the initial semesters, allowing students to lay a solid foundation for their practice.
The didactic coursework is paired with simulation laboratory courses and gradually increasing clinical experience in the general operating rooms of adult hospitals. By the fall semester, students are in the clinical setting up to three days a week, and up to four days a week by spring semester. In these settings, students hone the procedural skills learned in simulation labs and apply didactic theory while providing anesthesia for intra-abdominal, minor vascular, otolaryngological, dental, ophthalmological, gynecological, orthopedic, and outpatient surgical procedures.
First Year Learning Objectives and Outcomes
The intention of the first year is to indoctrinate students into the patient care environment. While clinical exposure increases gradually over time, it is important to note that CWRU MSA students are in the operating room almost immediately. Clinical exposure begins after a three-week “Boot Camp” in which students are immersed in didactic instruction, lectures, and simulation labs. Developed by CWRU instructors, this unique approach enables students to get a firm footing in the operating room and enables them to feel confident entering the operating room during the first month of coursework.
Throughout the clinical experience, students learn to collaborate with and perform anesthetic management under the supervision of anesthesiologists, certified anesthesiologist assistants, senior anesthesia residents, and fellows. In the spring semester, students begin the most innovative portion of the CWRU MSA curriculum, which integrates advanced simulation skill labs with crisis management, Anesthesia Non-Technical Skills lab work, and our highly interactive Clinical Decision Making course. Together, these courses maximize students’ technical skills, test and improve their crisis management, and deepen their knowledge of anesthetic management.
MSA Program Second Year: Clinical
Second Year Coursework
The second year is also comprised of clinical, didactic and simulation coursework, with increasing emphasis on self-directed learning. Didactic lectures are presented in a seminar format, directed toward critical review of literature on selected topics, current trends, and specialization. Students also participate in journal club, weekly conferences, an Ethics and Law of Practice course, and simulation labs that emphasize crisis across specialties.
Second Year Clinical Rotations
Clinically, the second year is spent almost exclusively in specialty rotations. Mandatory specialty rotations include: ambulatory anesthesia cardiothoracic and cardiovascular anesthesia, intensive care and preoperative clinic, nerve block, neurosurgical anesthesia, obstetrical anesthesia, pediatric anesthesia, and trauma.
Second-year students also have the opportunity to complete elective rotations across the country. Students can complete up to five months of elective specialty training, setting them apart from other MSA program graduates nationwide when applying to specialty hospitals.
Second Year Learning Objectives and Outcomes
Throughout the second year, students are in the operating room up to six days per week and are expected to take overnight calls. Their schedule in these final semesters is comparable to that of a full-time certified anesthesiologist assistant.
At the completion of the program of study, CWRU MSA graduates are prepared to manage and monitor patients of all ages and acuity for anesthesia care in outpatient, cardiac, thoracic, obstetric, pediatric, neuro, trauma, vascular, and geriatric surgeries. Graduates are trained for perioperative care, and have honed professional skills that are key to collaborating with the anesthesia care team. Our training results in the providing of superior patient care and, ultimately, saves lives.
Series Courses
Several of the courses in the Master of Science in Anesthesia Program are structured as long-term series courses, meaning students are progressively challenged by core components that build on one another and on the clinical experience over the course of multiple semesters.
These series include:
Students are taught basic and applied human systems physiology with an emphasis on topics and areas of special concern to anesthetists. As the series progresses, students are introduced to advanced concepts such as hemodynamics and maternal and fetal physiology.
Students complete two courses in the applied physiology series, each worth three credits. The courses are offered annually, with the first section in the first-year fall semester and the second in the first-year spring semester.
A series of conferences presented by students that address both anesthetic theory as it relates to the clinical experience, and basic and major problems in anesthesia management. Medical and surgical history of individual patients and the outcomes of anesthesia and surgery are presented and discussed.
This series emphasizes evidence-based medicine, and asks students to analyze data to justify treatments used in clinical practice. Students learn to critically appraise the literature, evaluate diagnostic test performance, design clinical pathways and standards of care, and implement evidenced-based medicine findings in their own clinical or administrative setting.
Students complete four courses in the anesthesia clinical correlations series, each worth one credit. The courses are offered annually, in the fall and spring semesters.
Beginning with an orientation in the summer semester, students are introduced to the operating room with an emphasis on the fundamental procedures and techniques used in administering anesthetic. Patient management and technical skills are refined with close attention to the didactic coursework.
Over the course of the clinical experience, students are exposed to all of the clinical specialties of anesthesiology and earn certification in Basic Life Support (BLS), Advanced Cardiac Life Support (ACLS), and Pediatric Advanced Life Support (PALS).
At the end of five of the six semesters, students sit for a comprehensive clinical examination designed to prepare them for the certification exam, which is required for all graduates who intend to practice as CAAs and is prepared by the National Commission for Certification of Anesthesiologist Assistants in consultation with the National Board of Medical Examiners.
Students complete six courses in the anesthesia clinical experience series, with credits increasing each semester.
Students cover a series of topics in basic medical science with a special emphasis on the effect of anesthetics on normal physiology.
Students complete four courses in the anesthetic science series, each worth one credit. The courses are offered annually, in the fall and spring semesters.
Students are taught the proper balance between circuits and engineering concepts and the clinical application of anesthesia instrumentation. Monitors and devices used in the operating room are studied with respect to principles of operation, calibration, and interpretation of data. A hands-on laboratory is utilized to maximize direct contact to the instrumentation of the profession.
Students complete two courses in the patient monitoring and instrumentation series, each worth two credits. The courses are offered annually, with the first section in the first-year summer semester and the second in the first-year spring semester.
Students are introduced to pharmacodynamics, pharmacokinetics, uptake, distribution and action of the volatile and intravenous anesthetics, muscle relaxants, narcotics, hypnotics, and other pharmaceuticals used in the administration of anesthesia.
The series provides an overview of drug actions, interactions, metabolism, methods of administration, dosages, side effects, precautions, and contraindications. Students also learn the basis for the use of medicines in pharmacologic and adjunct therapy of specific diseases.
Students complete two courses in the pharmacology series, each worth three credits. The courses are offered annually, in the fall and spring semesters of the first-year.
Students are introduced to physiological model-based simulation using on-screen computer simulation and mannequins. Emphasis is placed on improving appropriate anesthesia-related basic science knowledge, manual skills, drug and equipment setup, safety inspections, and performing anesthesia for uncomplicated surgical cases. As the series advances, students are introduced to crisis management and rescue techniques.
Students will also review and practice concepts vital to Basic Life Support and Advanced Cardiac Life Support, in which they earn certification through the anesthesia clinical experience series.
Students complete four courses in the physiological model-based simulation series, each worth one credit. The courses are offered annually, in the fall and spring semesters.
A complete overview of the courses for graduate students in the Master of Science in Anesthesia Program can be reviewed here. The curriculum is specifically designed for training the certified anesthesiologist assistant professional. Although other coursework may be similar, the MSA Program offers courses with a unique emphasis in anesthesia and the anesthesia care team model, as defined by the American Society of Anesthesiologists. All MSA students must follow the entire course curriculum. No exceptions will be made, regardless of degrees or certifications received, prior experience, work background, or education.
Courses are reserved for MSA students, and cannot be taken by other undergraduate or graduate students at the university.