When I was first applying to MSA programs, I asked every program if they had any medical missions or global health initiatives on my interview day. Many programs have a fundraising component like CWRU where they donate money to organizations to purchase equipment for patients abroad. While this is crucial in the global health landscape, I was also looking for an opportunity to be more hands on with the direct provision of healthcare.
CWRU has one of the only Master of Science in Anesthesia programs that supports medical mission trips for students that allows us to go abroad, do anesthesia in the operating room, and receive credit for the clinical experience. In Washington, D.C., the Program partners with the Medical Mission of Mercy (MMOM). This revelation drove a large part of my decision-making when it was time to decide where I wanted to train to become an anesthetist.
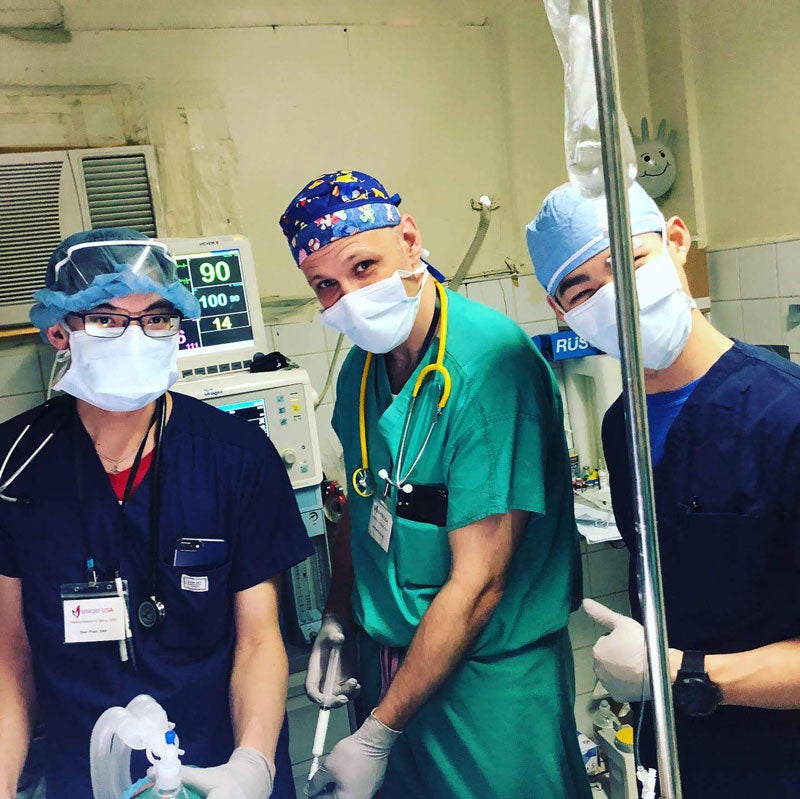
In January 2019, I traveled with the MMOM team, including two fellow MSA students, to the Philippines on my first medical mission.
The purpose of MMOM is to provide free medical services and medications to the underprivileged countries. Additionally, the organization has a long-term goal: to further educate healthcare providers who may otherwise not have access to additional education and training. The services provided are incredibly broad, and include:
- medical and surgical interventions, such as cleft lip or palate surgery, general surgery, and plastic surgery
- dental care, including extractions, fillings, root canals, and cleaning
- optometric care, such as eye exams, cataract screening, and providing prescriptions for glasses
- rehabilitation and wellness education, focused on women’s health, physical therapy, nutrition education, or injury prevention
Anesthesia is inextricably linked to surgical intervention and, on occasion, dental care. So, the anesthesia providers played an essential role for these two types of services provided by MMOM.
While in the Philippines, I worked alongside anesthesiologists who conducted pre-op examinations for patients undergoing surgery to ensure they were optimized for their upcoming procedure in addition to preparing them for surgery based on ASA standard guidelines. Some cases I had were thyroidectomies, hernia repairs, parotidectomies, branchial cyst excisions, tonsillectomies, cholecystectomies, hemorrhoidectomies, cleft lip and palate repairs, and lipoma excisions.
Our goal was always the same—to provide as safe an anesthetic plan as possible that allows patients to move comfortably through the phases of surgery, from induction to the perioperative stage, through emergence. It’s much easier said than done, especially because we didn’t have access to our usual supply of medications and equipment that we’re accustomed to having in the United States.
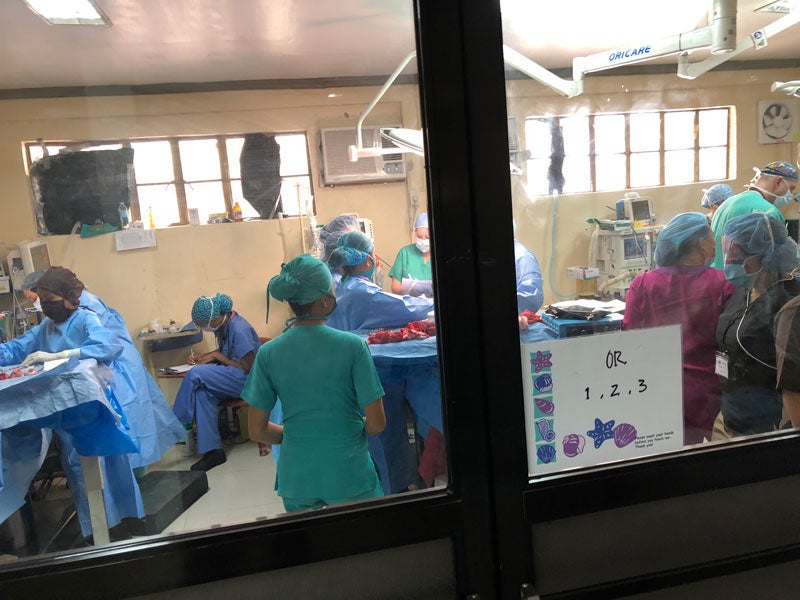
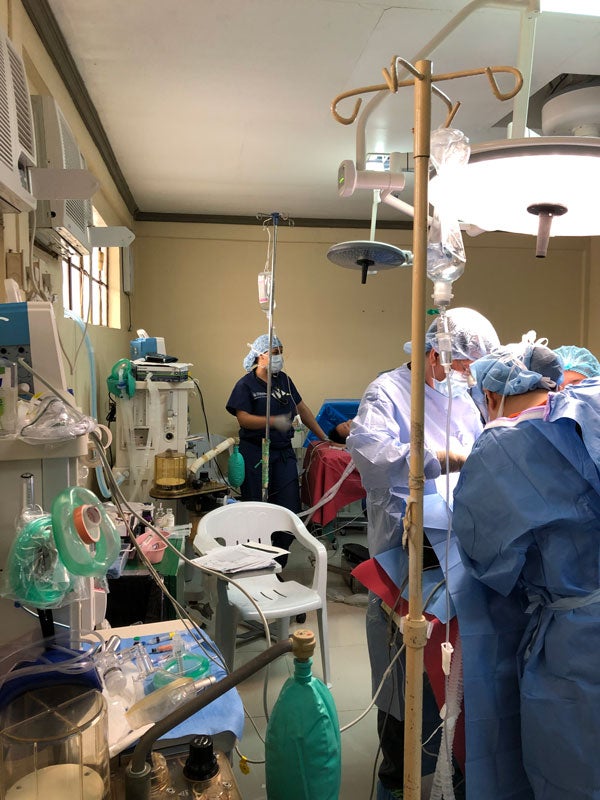
In fact, the limited supplies and the lack of standardization were what made the mission trip challenging. When urgent situations occurred, it was difficult to act quickly because each day we rotated to a different operating room, and it was like learning a new system.
Having said that, there was a calmness in the Philippines that does not exist at the hospital I currently train at in Washington, D.C. It was somewhat liberating to be able to practice anesthesia how it used to be practiced “back in the day,” when you bag-masked the patient until they came back to spontaneous ventilation. I like to call it “low-maintenance anesthesia.”
The caveat of course is that the patient population we served were predominantly healthier than the one I see during my clinical rotations in Washington, D.C. The population in D.C. that I serve is very sick, and training in that environment meant I was uniquely prepared for the medical mission. CWRU MSA does a tremendous job of throwing you into the deep end early on in your training, so the MSA students have seen a lot in just our first year of training. That’s not to say to “low-maintenance anesthesia” is necessarily easier—it’s a different challenge, but training in DC prepared me for the cases I saw. It’s not just the clinical exposure and familiarity with surgical procedures, but it’s also about the mental, emotional, and physical toll that long shifts have on you. These all play an important role in preparing you to practice anesthesia in unfamiliar environments.
The Impact of Medical Missions
Many of our surgical patients in the Philippines had very minimal interaction with the healthcare system. This is quite often the patient’s first medical treatment—and may have never seen a primary care physician or had experience with health insurance. The patients MMOM served were quite often marginalized and had minimal resources and financial capital.
I think that’s ultimately the role that MMOM plays in reducing health disparities because these patients would not have been able to afford these life-changing procedures otherwise. However brief our mission trip was, I believe that the impact of MMOM is far-reaching and has a direct and tangible effect on patients long after we leave.
As a student on this trip, I gained invaluable experiences while working in the Philippines. I gained autonomy in the operating room, and benefited from how much the anesthesiologist and anesthetists trusted students to manage cases intra-operatively.
Outside of the operating room, spending time with fellow volunteers was also invaluable. Coming from a social science background, I like to think of myself as a bit of an anthropologist. Here I was in a place thousands of miles away from home, but I didn’t feel homesick or suffer from culture shock. All the volunteers had something to contribute to MMOM. It didn’t matter if you were a clinician or not. Though we came from various backgrounds, we had a singular focus. The bond we share now is special, and it’s a privilege that not everyone is afforded. I will forever be grateful for this opportunity.
In the future, I would love to go on another medical mission trip. Before I started the MSA Program, I trained in public health with a focus on global health. I studied abroad in Denmark, Sweden, England, and Brazil. My interests at the time were primarily on the broader structural issues at the policy level.
Now, I envision myself taking that work a step further by combining my clinical training with global health policies, programs, and initiatives. I think it would be interesting to see how anesthesia, surgery, and medicine can contribute to regional stability in areas facing political turmoil, civil war, and humanitarian crises.
About the author: Dean Pham is currently a first-year student in the Master of Science in Anesthesia Program at Case Western Reserve University in Washington, D.C. Dean completed a bachelor’s degree in Ethnic Studies at The University of Texas at Austin and a master’s degree in Public Health at The University of Texas Health Science Center at Houston. After graduation, he worked as a research associate in pediatric surgery, where he was first exposed to anesthesia.