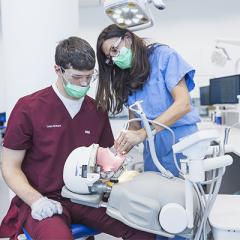
Inside the high-tech Simulation Clinic preparing students for real-world dental practice
Case Western Reserve University School of Dental Medicine’s Simulation Clinic emphasizes extensive hands-on training with state-of-the-art tools that reflect evolving clinical practices. The $2.6 million facility—funded largely through philanthropy and in-kind donations—allows students to practice procedures long before treating real people.
“We’re determined to be at the forefront of dental education,” said Kenneth Chance, DDS (DEN ’79), dean of the School of Dental Medicine. “Our objective is to ensure our students are ready to deliver high-quality care from their very first day with patients.

Case Western Reserve University School of Dental Medicine is now home to the Richardson Collection, a landmark study of longitudinal growth in 98 African-American children conducted by Elisha R. Richardson, BS, DDS, MS, PhD. The collection, including radiographs and dental casts, was entrusted to CWRU by Dr. Richardson’s family after his passing to ensure its preservation and accessibility for future generations of researchers.

Two hundred years after Case Western Reserve University’s founding, the School of Dental Medicine is shaping the future of dental education with bold vision and measurable progress. Guided by The Business of Dental Education, our comprehensive strategic plan approved in late 2023, we’ve spent the past two years transforming how we teach, learn, discover, and serve. From record-setting student achievement and groundbreaking research funding to innovative patient care models and expanded community partnerships, the milestones of 2024 and 2025 reflect both our tradition of excellence and our momentum for the future.
In this issue:
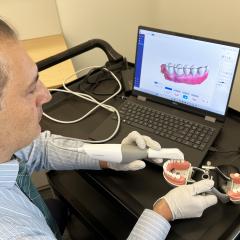
- Transforming how dentists are trained
- Newly renovated Simulation Clinic
- And much more!
Past issues of the magazine and issues of departmental newsletters are available in the archive.




